The State of Mental Health in America
Mental Health America (MHA) is committed to promoting mental health as a critical part of overall wellness. We advocate for prevention services for all, early identification and intervention for those at risk, integrated services, care and treatment for those who need them, and recovery as the goal.
We believe that gathering and providing up-to-date data and information about disparities faced by individuals with mental health problems is a tool for change.
Due to methodological and societal changes caused by the COVID-19 pandemic between 2019-2020, SAMHSA has announced that the 2019-2020 data from the National Survey on Drug Use and Health (NSDUH) survey may be misleading. Twelve of the 15 indicators used to rank the states in the 2023 State of Mental Health in America report were calculated using the 2019-2020 NSDUH data. We report this as a caution regarding interpretation of this year’s report and a reminder that the 2023 State of Mental Health in America report cannot be compared to previous or future reports. For more information, see SAMHSA’s statement here.
FILL OUT THE FORM BELOW TO DOWNLOAD THE PRINTABLE VERSION OF THE REPORT.
2023 Key Findings
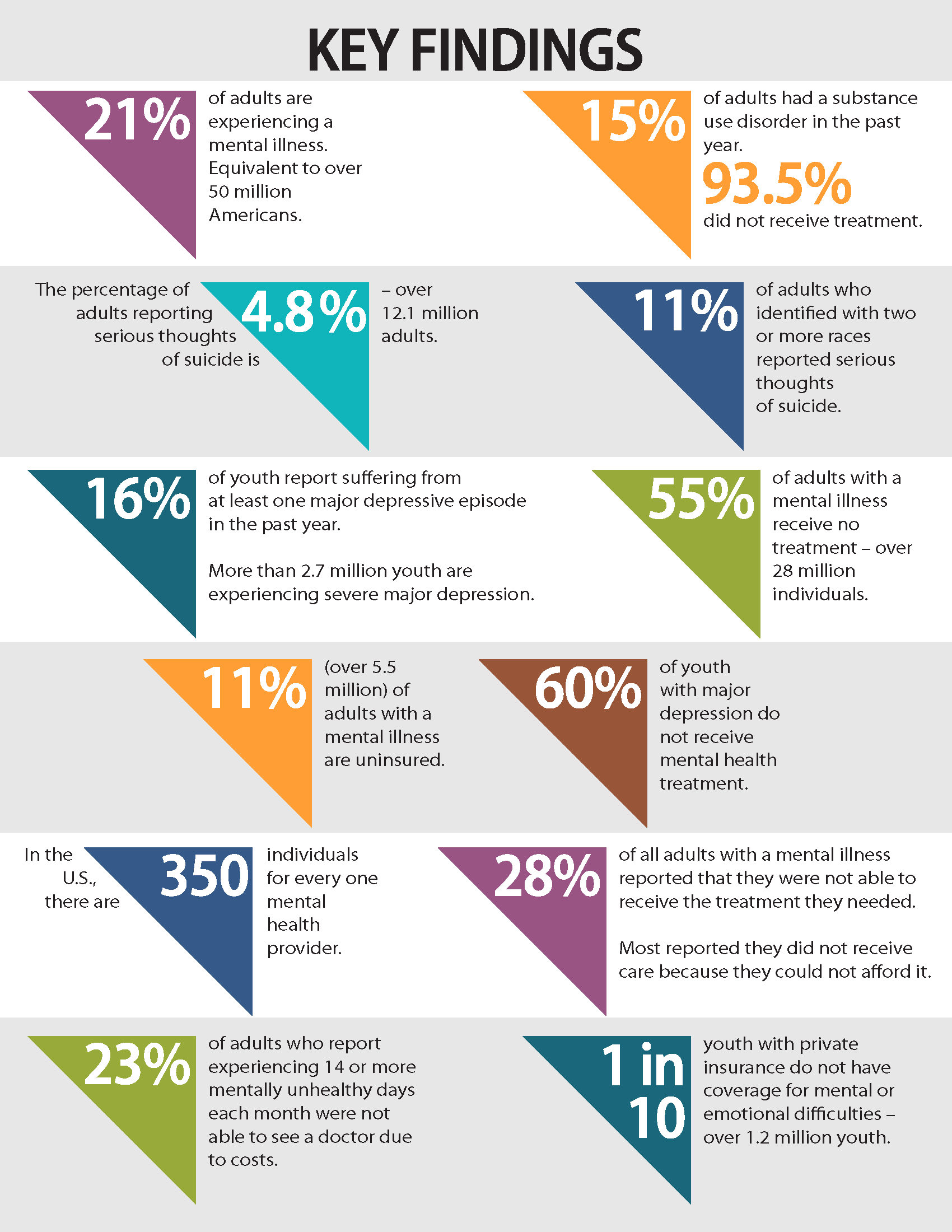
- In 2019-2020, 20.78% of adults were experiencing a mental illness. That is equivalent to over 50 million Americans.
- The vast majority of individuals with a substance use disorder in the U.S. are not receiving treatment. 15.35% of adults had a substance use disorder in the past year. Of them, 93.5% did not receive any form of treatment.
- Millions of adults in the U.S. experience serious thoughts of suicide, with the highest rate among multiracial individuals. The percentage of adults reporting serious thoughts of suicide is 4.84%, totaling over 12.1 million individuals. 11% of adults who identified with two or more races reported serious thoughts of suicide in 2020 – 6% higher than the average among all adults.
- Over 1 in 10 youth in the U.S. are experiencing depression that is severely impairing their ability to function at school or work, at home, with family, or in their social life. 16.39% of youth (age 12-17) report suffering from at least one major depressive episode (MDE) in the past year. 11.5% of youth (over 2.7 million youth) are experiencing severe major depression.
- Over half (54.7%) of adults with a mental illness do not receive treatment, totaling over 28 million individuals. Even in Montana (ranked #1), over 4 in 10 adults with a mental illness did not receive care.
- Almost a third (28.2%) of all adults with a mental illness reported that they were not able to receive the treatment they needed. 42% of adults with AMI reported they were unable to receive necessary care because they could not afford it.
- 10.8% (over 5.5 million) of adults with a mental illness are uninsured. Hispanic adults with AMI were least likely to have health insurance, with 19% reporting they were not covered by insurance.
- 6.34% of youth in the U.S. reported a substance use disorder in the past year. That is equivalent to over 1.5 million youth in the U.S. who meet the criteria for an illicit drug or alcohol use disorder.
- 22.87% of adults who report experiencing 14 or more mentally unhealthy days each month were not able to see a doctor due to costs. In Georgia (ranked 51), over one-third of adults experiencing frequent mental distress are unable to afford a doctor’s visit.
- 59.8% of youth with major depression do not receive any mental health treatment. Asian youth with major depression were least likely to receive specialty mental health care, with 78% reporting they did not receive mental health services in the past year. In South Carolina, the lowest ranking state, nearly 8 in 10 youth with depression do not receive care.
- Nationally, only 28% of youth with severe depression receive some consistent treatment (7-25+ visits in a year). Most (57.3%) youth with severe depression do not receive any care.
- Nationally, 1 in 10 youth who are covered under private insurance do not have coverage for mental or emotional difficulties – totaling over 1.2 million youth. In Arkansas (ranked 51), nearly one-quarter of youth with private insurance do not have coverage for mental health care.
- Only .718 percent of students are identified with emotional disturbance for an individualized education program (IEP). IEPs, with sufficient resources for schools and teachers, are critical for ensuring that youth with disabilities can receive the individualized services, supports, and accommodations to succeed in a school setting.
- In the U.S., there are an estimated 350 individuals for every one mental health provider. However, these figures may actually be an overestimate of active mental health professionals, as it may include providers who are no longer practicing or accepting new patients..
Explore the web-based report using the links provided on the left or download the printable report.
The State of Mental Health in America
In the above links you will find a Collection of Data across all 50 states and the District of Columbia answering the following questions:
- How many adults and youth have mental health issues?
- How many adults and youth have substance use issues?
- How many adults and youth have access to insurance?
- How many adults and youth have access to adequate insurance?
- How many adults and youth have access to mental health care?
- Which states have higher barriers to accessing mental health care?
Our Goal:
- To provide a snapshot of mental health status among youth and adults for policy and program planning, analysis, and evaluation;
- To track changes in the prevalence of mental health issues and access to mental health care;
- To understand how changes in national data reflect the impact of legislation and policies; and.
- To increase dialogue and improve outcomes for individuals and families with mental health needs
Why Gather this Information?
- Using national survey data allows us to measure a community’s mental health needs, access to care, and outcomes regardless of the differences between the states and their varied mental health policies.
- Rankings explore which states are more effective at addressing issues related to mental health and substance use.
- Analysis may reveal similarities and differences among states in order to begin assessing how federal and state mental health policies result in more or less access to care.
This publication was made possible by the generous support of Alkermes and Otsuka America Pharmaceutical Companies.

The content of this webpage is the property of Mental Health America. MHA grants a limited license to use the webpage, or portions thereof, only if, whenever the webpage is used in written or electronic form, it is clearly stated that the website was created by and is the property of Mental Health America and a link is provided to www.mhanational.org. Under no circumstances may the website be used for any commercial purpose without the express written permission of Mental Health America. For permission to use the content of this webpage, please contact info@mhanational.org.


